Surgical Treatments
For men that suffer from persistent incontinence, there are long-term treatments available. Talk to your doctor or urologist to explore whether this option is right for you.
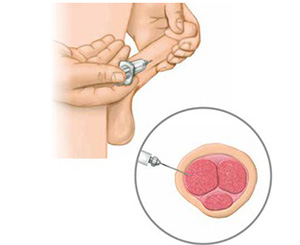
Injection Therapy
Injection of bulk producing agents, such as collagen, can be used to help control urine leakage from a weak urinary sphincter. The material is injected into the wall of the urethra, bulking up the tissue and causing it to tighten. Material can also be injected into the tissues surrounding the sphincter and urethra to provide additional resistance.2 The material that is injected into the tissues help to provide closure of the urethra and make it more difficult for urine to leak out.1
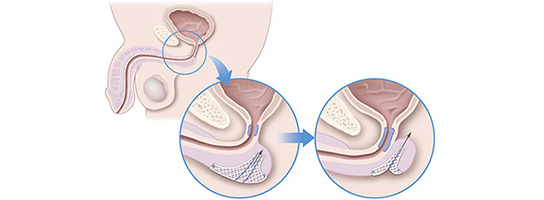
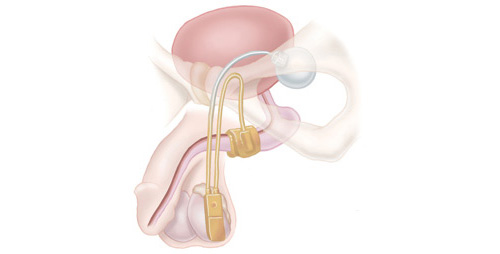
Male Pelvic Sling
The male pelvic sling is designed to stop leakage by supporting the sphincter muscle. The sling is a strip of soft mesh placed inside the body through small openings that are made to access the urethra and the urinary sphincter. The male sling moves the sphincter back to its natural position to help restore bladder control and provide continence. It requires no action by the patient to function and most patients are continent immediately following the procedure.6
At their urologist’s discretion, many patients can resume non-strenuous activity within a few days and normal daily activities six weeks later.7
Benefits:
Risks and Side Effects:7
As with any medical procedure, complications may occur. Some risks include, but are not limited to; device failure, urinary retention, post-operative pain, irritation at the wound site and foreign body response.
Benefits and risks associated with a male sling
Explains the difference between the male sling and artificial urinary sphincter.
Who is a candidate for a male sling?
Take the Quiz
Take our quiz to identify if you are experiencing urinary incontinence symptoms and help kick-start the conversation with your doctor.
Questions to Ask
Helpful hints on how to start the conversation with your GP or urologist, and other useful resources.
References
- Medline Plus. (n.d.). Retrieved December 13, 2019, from https://medlineplus.gov/ency/article/007373.htm.
- National Association for Continence. (n.d.). Retrieved December 13, 2019, from https://www.nafc.org/male-products.
- AMS 800™ Urinary Control System Operating Room Manual. American Medical Systems, Inc. 2011
- Poole K, Kerlin M, Wynne R. Prevalence and characteristics of urinary incontinence in a cohort of patients with chronic heart failure. Heart Lung. 2017; 46 (2): 67-73. https://www.heartandlung.org/article/S0147-9563(16)30224-2/fulltext
- Montague D. K. (2012). Artificial urinary sphincter: long-term results and patient satisfaction. Advances in urology, 2012, 835290. doi:10.1155/2012/835290
- Welk BK. Herschorn S. The male sling for post-prostatectomy urinary incontinence: a review of contemporary sling designs and outcomes. Br J Utol Int. 2011;109:328–344.
- AdVance™ Male Sling System Instructions for Use. American Medical Systems, Inc. 2010.
- Rehder P, Haab F, Cornu JN, et al. Treatment of post-prostatectomy male urinary incontinence with the transobturator retroluminal repositioning sling suspension: 3-year follow up. Eur Urol. 2012 Jul;62(1):140-5.
- Sturm RM, Guralnick ML, Stone AR, et al. Comparison of clinical outcomes between “ideal” and “nonideal” transobturator male sling patients for treatment of post prostatectomy incontinence. Urol. 2014 May;83(5):1186-8.
Results from case studies are not necessarily predictive of results in other cases. Results in other cases may vary. All images are the property of Boston Scientific. All trademarks are the property of their respective owners.
Disclaimer: Individual symptoms, situations, circumstances and results may vary. This information is not intended to be used for medical diagnosis or treatment or as a substitute for professional medical advice. Please consult your doctor or qualified healthcare provider regarding your condition and appropriate medical treatment.
These Videos are meant for informational purposes only and may not be indicative of clinical outcome. The opinions, procedures and patient care policies expressed or depicted in the videos are those of the physician or practice nurse and do not necessarily reflect the opinions, policies or recommendations of Boston Scientific Corporation or any of its employees.
This site is intended for Australian residents only. Please review the Boston Scientific Privacy Policy, for practices on the collection, storage, use and disclosure of your personal information.
CAUTION : Indications, contraindications, warnings and instructions for use can be found in the product labelling supplied with each device.